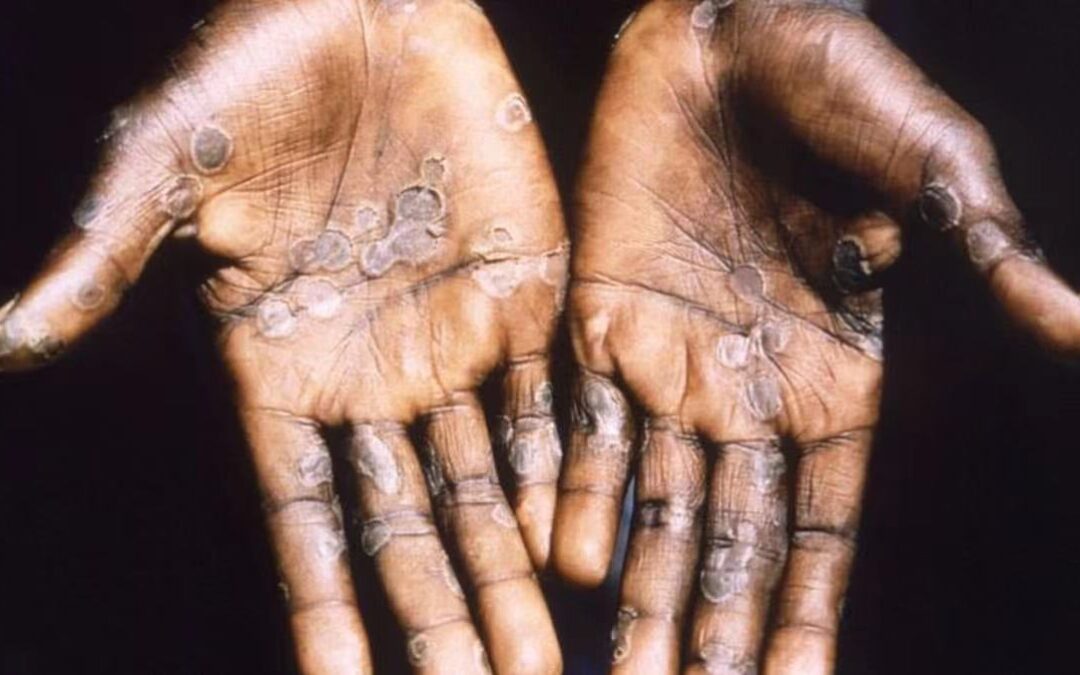
Risk assessment of Monkeypox
ECDC
Monkeypox (MPX) does not spread easily between people. Human-to-human transmission occurs through close contact with infectious material from skin lesions of an infected person, through respiratory droplets in prolonged face-to-face contact, and through fomites. The predominance, in the current outbreak, of diagnosed human MPX cases among men having sex with men (MSM), and the nature of the presenting lesions in some cases, suggest transmission occurred during sexual intercourse.
Based on ECDC’s epidemiological assessment, the likelihood of MPX spreading in persons having multiple sexual partners in the EU/EEA is considered high. Although most cases in current outbreaks have presented with mild disease symptoms, monkeypox virus (MPXV) may cause severe disease in certain population groups (young children, pregnant women, immunosuppressed persons). However, the likelihood of cases with severe morbidity cannot be accurately estimated yet. The overall risk is assessed as moderate for persons having multiple sexual partners (including some groups of MSM) and low for the broader population.
Treatment is mainly symptomatic and supportive, including prevention and treatment of secondary bacterial infections. Smallpox vaccine can be considered for post-exposure prophylaxis of close contacts at increased risk for severe disease, however careful benefit/risk assessment should be performed for the exposed individual. Important information on the use of currently available smallpox vaccines is missing for groups at increased risk for severe disease. In addition, antivirals are potential treatment options for severe cases.
EU/EEA countries should focus on prompt identification, management, contact tracing and reporting of new MPX cases. Countries should update their contact tracing mechanisms, their diagnostic capacity for orthopoxviruses and review the availability of smallpox vaccines, antivirals and personal protective equipment (PPE) for health professionals.
An interim case definition is proposed for case reporting. Guidance for the management of MPX cases and close contacts is also included. Cases should remain isolated until their rash heals completely, avoiding contact with immunosuppressed persons and pets. Abstaining from sexual activity and close physical contact is also advised until the rash heals. Most cases can remain at home with supportive care.
Close contacts of MPX cases should self-monitor for the development of symptoms up to 21 days from the last exposure to a case. Healthcare workers should wear appropriate PPE (gloves, water-resistant gown, FFP2 respirator) when screening suspected cases or caring for a MPX case. Laboratory personnel should also take precautions to avoid occupational exposure. Close contacts of a MPX case should be deferred from blood, organ or bone marrow donations for a minimum of 21 days from the last day of exposure.
Proactive risk communication and multiple community engagement activities should be carried out to increase awareness, provide updates and guidance to those at increased risk and the wider public. Risk communication messages should stress that MPXV is spread through close contact between people, especially in the same household, potentially including the sexual route. A balance should be kept between informing those most at risk but also communicating that the virus does not spread easily between people the risk to the broader population is low.
There is a potential risk of human-to-animal transmission in Europe, therefore close intersectoral collaboration between human and veterinary public health authorities working from a ‘One Health’ perspective is needed to manage exposed pets and prevent the disease from being transmitted in wildlife. EFSA is not aware to date of any reports on infections in animals (pets or wild animals) in the EU.